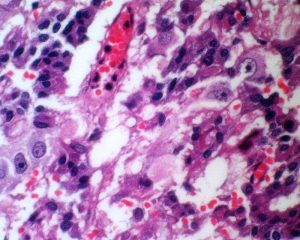
 These lesions originate in a part of the hypophysis, the adenohypophysis, a gland that secretes hormones that regulate body functions. In a large majority of cases they are benign lesions, but as they interfere with hormonal mechanisms and the compressive effect they may have on adjacent structures, they should be treated.
These lesions originate in a part of the hypophysis, the adenohypophysis, a gland that secretes hormones that regulate body functions. In a large majority of cases they are benign lesions, but as they interfere with hormonal mechanisms and the compressive effect they may have on adjacent structures, they should be treated.
Clinical signs
Depending on the type of hormone segregated by the tumour, in the event of the functioning tumours, there are several possible clinical profiles. In the majority of cases the tumours are non-secreting, that is the tumour itself does not produce any hormone, and so the clinical signs will be those of the absence of hormonal action, in other cases there is excess prolactin, and in others of growth hormone. This is called acromegaly or cortisol in Cushing’s syndrome.
Diagnostic tests
In these patients apart from the imaging tests common to all brain tumours, analytical determinations should be made to determine the current hormonal situation of the patient. These tests should then be repeated following surgery to assess its repercussion on hormonal secretion in those cases where the tumour produced a specific type of hormone.
Treatment
The first approach should be pharmacological. Cases presenting poor response to medical treatment should be remitted to surgical treatment. Surgery should not be delayed in patients suffering visual disorders as de deficiencies may become permanent.


 These lesions originate in a part of the hypophysis, the adenohypophysis, a gland that secretes hormones that regulate body functions. In a large majority of cases they are benign lesions, but as they interfere with hormonal mechanisms and the compressive effect they may have on adjacent structures, they should be treated.
These lesions originate in a part of the hypophysis, the adenohypophysis, a gland that secretes hormones that regulate body functions. In a large majority of cases they are benign lesions, but as they interfere with hormonal mechanisms and the compressive effect they may have on adjacent structures, they should be treated.